
Why Your Allergy Medication Is Not Solving the Real Problem
Your Medication Is Working. So Why Do You Still Feel Terrible?
Allergy medications like antihistamines and nasal sprays can quiet symptoms, but they do not fix the reason your immune system keeps reacting. If your symptoms come back as soon as the medicine wears off, or you still feel foggy, tired, and miserable despite doing everything right, it may be time to look beyond symptom management. This post explains why that cycle happens, how it affects your quality of life, and what a root-cause approach to allergy care can look like.
Key Takeaways:
Symptom relief is not treatment. Antihistamines quiet the reaction but don't change why it keeps happening.
The cycle is a design limitation, not your fault. Symptoms return because the underlying immune response never stops.
Allergies affect your whole life. Fatigue, brain fog, and poor sleep are real consequences, not just congestion.
Medication side effects can make things worse. Dryness, cognitive dullness, and fatigue layer on top of existing symptoms.
Kansas is especially brutal for allergy sufferers. Overlapping pollen seasons mean months of continuous exposure.
Root-cause care changes the question. The goal is immune retraining, not just symptom suppression.
If you are taking allergy medicine and still feeling miserable, you are not alone. And you are not doing anything wrong.
I see this constantly.
People come in having already tried the antihistamines, the nasal sprays, the early-season dosing. They are doing everything they were told to do. They are being responsible. They are trying. And they still feel foggy, congested, inflamed, and worn down every single allergy season like clockwork.
That is not a personal failure. That is a gap in how allergies are typically treated. At Everyday Wellness, we approach things differently.
Here is the truth most people are never told directly: symptom relief is not the same thing as treatment.
That one distinction changes everything. Once you understand it, the frustration of doing "all the right things" and still feeling awful finally starts to make sense.
What Is Actually Happening in Your Body
To understand why medication alone often falls short, it helps to understand what is actually going on when your allergies flare.
Your immune system is designed to protect you. When it encounters something it considers a threat, it launches a defense. For people with environmental allergies, the immune system has essentially made a mistake. It has been decided that something harmless, like pollen, grass, mold, or dust mites, is a danger. So every time you come into contact with that trigger, your immune system responds as if it needs to fight something off.
Part of that response involves a chemical called histamine. When your immune system activates, specialized cells release histamine into your tissues. Histamine causes blood vessels to expand, mucus production to increase, and nerve endings to become more sensitive. The result is the combination most allergy sufferers know well: sneezing, runny nose, itchy eyes, congestion, sinus pressure, and headaches.
But for many people, the response does not stop there.
Histamine also affects the brain and the rest of the body. It can disrupt sleep quality, contribute to persistent fatigue, and create that heavy, foggy feeling that makes it hard to think clearly or stay motivated. Some people describe it as feeling like they are moving through water. Others say they just feel off, like they are not quite themselves during allergy season.
That is not in your head. That is your immune system doing exactly what it was designed to do. It just happens to be doing it in response to the wrong thing.
When you take an antihistamine, you are introducing a medication that blocks histamine receptors. That means histamine is still being released, but your body cannot respond to it as strongly. The symptoms quiet down. You feel better, at least for a while.
That is genuinely useful. I want to be clear about that.
But here is what the antihistamine is not doing. It is not telling your immune system to stop reacting to pollen. It is not retraining your body to recognize grass as harmless. It is not changing anything about the underlying immune response that is triggering the problem.
The alarm is still going off. You have just turned down the volume.
Why Symptom Control Becomes a Cycle
This is where things get frustrating for a lot of people.
Because the medication is managing the reaction rather than changing it, the moment the medication wears off, your immune system picks right back up where it left off. The trigger is still there. Your immune system still considers it a threat. The symptoms return.
So most people do what makes sense. They take the medication again.
Over time, that pattern becomes the new normal. You take it every day during allergy season. Maybe you start taking it earlier each year. Maybe you add a nasal spray on top of it. Maybe you try a different antihistamine when the first one stops feeling as effective. And at some point, you realize you have been managing this the same way for years, and nothing has actually changed.
That cycle is incredibly common. And I want you to understand why it happens, because it is not because you are doing something wrong. It is because the tools most people have access to are only designed to do one thing: manage the symptoms of a reaction that keeps happening.
What they are not designed to do is change the reason the reaction keeps happening in the first place.
That is a very different goal. And it requires a very different approach.
The Hidden Cost of Living in Allergy Management Mode

One thing I notice with patients who have been managing allergies for a long time is that they often forget what it feels like to not be managing them.
They have adjusted their baseline. They have gotten so used to functioning at 70 or 75 percent that they think that is just how they are. They chalk up the fatigue to being busy. They attribute the brain fog to stress. They assume the disrupted sleep is just part of getting older. And they push through allergy season every year because that is what they have always done.
But when we actually sit down and talk through how they feel day to day during peak allergy periods, the picture becomes much clearer.
The fatigue is real. Chronic low-grade inflammation takes energy. Your body is working overtime running an immune response that was not necessary in the first place, and that costs you. It shows up as tiredness that does not improve with sleep. It shows up as needing more caffeine to get through the afternoon. It shows up as not wanting to exercise or go outside because you already feel run down.
The brain fog is real. Histamine has a direct effect on the central nervous system. When your immune system is activated repeatedly over weeks or months, it can affect focus, memory, processing speed, and mood. Some people notice they are more irritable during allergy season. Some struggle to concentrate at work. Some feel emotionally flat or just harder to be around. And for women in midlife, it is worth knowing that hormones can make this even more complicated. If you have ever wondered whether your allergy symptoms might have a hormonal component, this post on the connection between allergies and hormone health is worth reading.
The sleep disruption is real. Congestion makes it harder to breathe at night. Histamine in the brain can interfere with sleep cycles. Poor sleep compounds everything else: the fatigue, the brain fog, the irritability, and the reduced ability to cope with daily demands.
And none of that is being addressed by taking an antihistamine in the morning.
I am not saying this to be discouraging. I am saying it because most people have never had someone explain to them what is actually happening in their body and why it affects so much more than just their sinuses.
You deserve that explanation. You deserve to know that what you are experiencing is real, that it has a cause, and that there are approaches designed to address more than just the surface level.
The Side Effects Nobody Talks About Enough
There is another layer to this conversation that does not get enough attention.
Antihistamines help many people. But they also come with a set of side effects that, for some patients, create their own set of problems on top of the allergy symptoms they were already dealing with.
The most common issue is dryness. Antihistamines work partly by reducing secretions, and that affects more than just your nasal passages. Many people experience dry mouth, dry eyes, dry skin, or a persistent feeling of thirst that is hard to satisfy. For people who already deal with dry eyes or dry skin as a separate concern, this can make things noticeably worse.
Some people experience constipation on antihistamines. Some experience urinary hesitancy or difficulty, particularly older adults or people who are already sensitive to medications. Some people feel drowsy, even on medications marketed as non-drowsy. Others feel oddly wired and have trouble sleeping. And some people notice cognitive effects: a kind of dullness or slowness that sits on top of the brain fog they were already experiencing from the allergies themselves.
So now the picture is this: you still have allergy symptoms, and the medication meant to help is contributing its own layer of physical discomfort.
I want to say clearly again that this does not mean antihistamines are bad medications. They have a real place in allergy care. But it does mean that for some patients, the side effect profile makes them a poor long-term solution. And for patients who are already dealing with fatigue, brain fog, and feeling run down, adding more of those sensations through medication side effects is a real problem.
If you have ever felt like you were choosing between allergy symptoms and medication side effects, that is a sign that the current approach is not a good enough fit for your body.
You deserve a better option than that.
Why Kansas Makes This Harder Than Most Places
Here in Kansas, allergies are not just a seasonal inconvenience. They are a serious, persistent quality of life issue for a significant portion of the population.
Wichita consistently ranks among the worst cities in the nation for allergy sufferers, with some of the highest tree, grass, and weed pollen levels in the country. We have wind. We have open land. We have a climate that supports long pollen seasons. And because of the geography of this region, there is not much to buffer the movement of airborne allergens from one area to the next.
For many of my patients, allergy season is not a few rough weeks. It is multiple months of overlapping triggers where one season bleeds into the next. Tree pollen in the spring transitions into grass pollen in late spring and early summer, which transitions into weed pollen and mold in late summer and fall. Indoor allergens like dust mites do not have a season at all.
That means some patients are managing symptoms for the better part of the year.
When allergy exposure is that continuous, a strategy built only on symptom management is almost guaranteed to feel inadequate. You are constantly reacting. You are constantly medicating. And you never really get ahead of it.
That is exactly why I believe people in this region need access to a more complete conversation about allergy care, one that includes options beyond managing the reaction over and over again for the rest of their lives.
What Root-Cause Allergy Care Actually Means
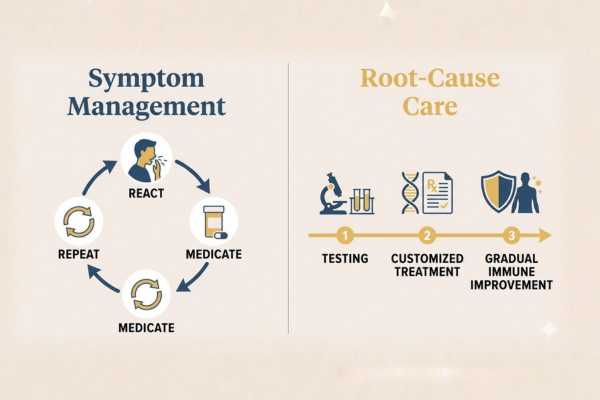
When I talk about root-cause care, I mean asking a different question entirely.
Not just: "What can I take to feel better today?"
But also: "Why is my body reacting like this, and can we actually help it respond differently over time?"
Those are two very different goals. The first is about managing what is happening. The second is about changing it.
Root-cause allergy care starts with getting a clearer picture of what is actually driving the problem. That means looking at your symptom history in detail. When do your symptoms tend to flare? Are they seasonal or year-round? Are there specific environments or situations that make things worse? What have you tried, and how did your body respond? Are you still suffering even while medicated?
Testing helps fill in the picture. Instead of guessing which environmental triggers might be affecting you, testing gives us something concrete to work with. It identifies the specific things your immune system is reacting to so that care can be built around your actual pattern rather than a general assumption.
From there, the goal shifts from reaction management to immune retraining.
That is a concept worth sitting with for a moment. The objective is not to silence the immune response. The objective is to help the immune system learn to recognize specific triggers differently so the reaction becomes less intense over time.
That is not something a daily antihistamine can do. It requires a different kind of intervention, one that works with the immune system rather than simply blocking its signals. You can learn more about how we approach Allergy Management at Everyday Wellness and what that process looks like.
Why This Matters for Your Quality of Life
I want to step back for a moment and talk about why any of this matters beyond just feeling less congested.
Allergies affect how you show up in your life. They affect how much energy you have for your family. They affect your ability to focus at work. They affect whether you want to go outside with your kids or stay in because you know how you will feel afterward. They affect your sleep, your mood, your patience, and your sense of well-being.
When allergies are poorly controlled, people often quietly withdraw from things they used to enjoy. They stop planning outdoor activities around peak pollen season. They turn down invitations because they know they will feel terrible. They cancel plans because the fatigue from a bad allergy day made it impossible to follow through.
That is a real quality of life cost, and it tends to build slowly enough that people do not always notice how much they have given up.
I care about this because I do not think you should have to organize your life around avoiding allergy triggers. I do not think you should have to plan your energy around when your medication will wear off. And I do not think you should have to accept that this is just how every spring and fall is going to feel for the rest of your life.
Especially not when there may be a more complete path forward.
Signs It May Be Time to Look Deeper
If any of these sound familiar, it may be time for a different kind of conversation:
You take allergy medication regularly and still have bad days
Your symptoms return reliably as soon as the medication wears off
You have breakthrough flares even while actively medicated
You do not tolerate antihistamines well, or the side effects are their own problem
You feel tired, foggy, congested, or just off throughout allergy season
You feel like you are functioning at a lower level than you should be for weeks or months at a time
You want to understand what is actually triggering your immune system
You are ready for a plan that looks further ahead than getting through the next 24 hours
This does not mean you have done anything wrong by using medication. It does not mean antihistamines have no value. It simply means you may be ready to ask a more complete question about your care.
My Perspective as Both a Provider and a Patient
Part of why I care so much about this is personal.
I have dealt with severe allergies myself. I know what it is like to feel genuinely miserable. I know what it is like to have symptoms interfere with your ability to think, work, and be present. And I know what it feels like to want something that actually changes the pattern instead of just getting you through another day.
That experience shaped how I approach allergy care for my patients.
I want people to understand what their body is doing. I want them to know when a treatment is offering temporary relief and when an approach is actually designed to work at a deeper level. And I want them to have access to options that are realistic for real life, not just effective on paper.
Too many people have been told, either directly or implicitly, that managing symptoms is the best they can do. I do not believe that is true for most patients. And I think that if you have been suffering through allergy season year after year, you deserve to at least have a real conversation about whether there is a better path.
You Do Not Have to Keep Settling
If you have been pushing through allergy season on medication for years and wondering whether there is something more, the answer may be yes.
You deserve to understand what is actually going on in your body. You deserve a care approach that looks at more than how to quiet your symptoms for a few hours. And you deserve to make informed decisions about your health based on a full picture, not just the options that are easiest to reach for.
At Everyday Wellness, I take time with each patient to look at their symptoms, their history, and their testing so we can decide together what approach makes the most sense for them. That is not a one-size-fits-all conversation. Every person reacts differently, tolerates different things, and has different goals for their health.
But the starting point is always the same: understanding what is actually driving the problem.
If you are tired of managing symptoms and ready to ask a better question about your allergy care, I would love to talk with you.
Call (316) 391-3465, visit https://everydaywellnesswichita.com/contact, or email [email protected] to schedule a consultation.
You do not have to keep white-knuckling your way through allergy season. Let us figure out what your body has been trying to tell you.
This article is for educational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Please consult your qualified healthcare professional before making any changes to your care.


